If you’ve had a hysterectomy, you may be concerned about rapid aging post-surgery. Some women notice changes in their skin and hormonal changes as well. All this leads to concern and the question of whether hysterectomy causes premature aging. As with any other surgical procedure, there are many factors that affect hysterectomy outcomes. For this reason, let’s consider hysterectomy in depth.
What Is a Hysterectomy?
A hysterectomy is a surgical procedure in which your uterus and/or your ovaries are removed. As with any other surgical procedure, hysterectomy demands incisions to be made to your body and a recovery period of 4-6 weeks. If you have a hysterectomy or are preparing to have one, you should consult with your surgeon about any risks associated with the procedure, as well as the recovery period.
Both your surgeon and your GP can help you understand the recovery period better. They can also help you better understand the likelihood of rapid aging after this procedure, as well as ways to limit the aging. You should also understand the importance of physical activity and how its rejuvenating effects can help you reduce the rapid aging rate.
Types of Hysterectomy
Depending on the reasons your doctor suggests a hysterectomy, you may have either: an abdominal or vaginal hysterectomy. Besides this, there are factors that can affect the scope of your hysterectomy. As this is the second most-performed hysterectomy procedure for women, over time, multiple types of hysterectomy have been developed:
- Partial hysterectomy,
- Total hysterectomy, and
- Radical hysterectomy.
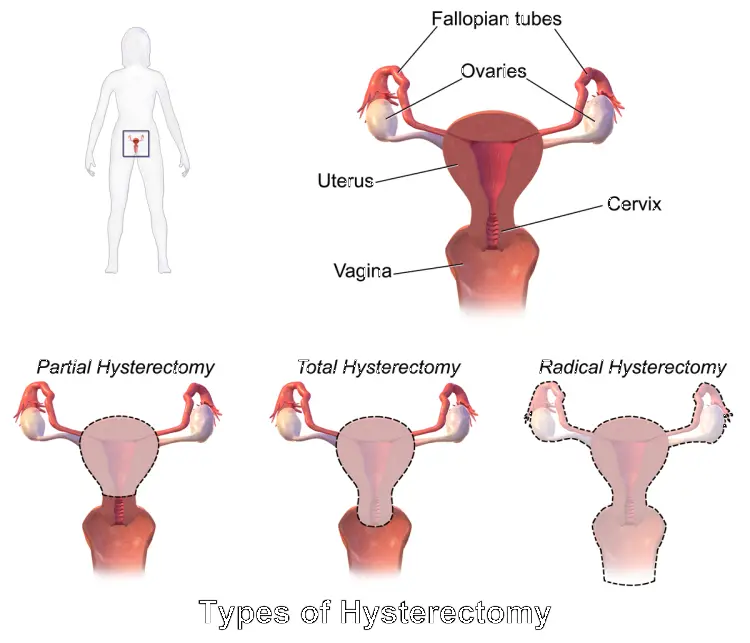
Partial Hysterectomy
In partial hysterectomy, the uterus only is removed. A partial hysterectomy is a procedure that does not touch your vagina or the cervix. Your ovaries are also left in place. For this reason, since your ovaries are not removed, they can still produce estrogen. Women who have partial hysterectomy do not experience surgical menopause after partial hysterectomy. However, only 22% of hysterectomy procedures are partial.
Total Hysterectomy
In a total hysterectomy, the entire uterus and the cervix are removed. If the ovaries are kept in place, you will not experience surgical menopause post total hysterectomy. As this procedure is more invasive (it removes more of your tissue), you may experience a slightly longer recovery time, depending on your age and overall health status.
Radical Hysterectomy
Radical hysterectomy includes the removal of the uterus, cervix, the upper portion of your vaginal canal, and, in most cases, ovaries as well. Most doctors suggest that during this procedure, your ovaries are removed as well since if left in place, you risk developing ovarian cancer. For this reason, your doctor will perform salpingo-oophorectomy – the removal of the ovaries. In any case, once your ovaries are removed, you will undergo immediate menopause (surgical menopause) and will not ovulate anymore.
Why Would You Need a Hysterectomy?
Hysterectomy is one of the most common procedures for women in the US. It is a single procedure that may be done if:
- You have ovarian fibroids,
- Your experience severe pelvic pains (as a result of Pelvic Inflammatory Disease, Fibroids, or Adenomyosis),
- You experience the prolapse of the uterus or have
- Cancer of the womb (the uterus), ovaries, or cervix.
Hysterectomy can significantly improve the quality of your life. It can also save a life in some cases, such as in cancer patients or after accidents, when there is heavy bleeding from the uterus that cannot be stopped fast enough. In most cases, however, you will have a chance to talk over the procedure with your doctor, and you will know why a hysterectomy is done and what you can expect during the recovery period.
What to Do if You Are Considering a Hysterectomy?
In some cases, however, hysterectomy can be voluntary. Many women who have had a problematic uterus, a history of repeated pelvic inflammatory disease, or cases of cervical or ovarian cancer or cancer of the uterus in the family decide to remove their uterus as a measure of precaution. This can mean consulting with your family doctor or a specialized surgeon, as well as a series of tests and anamnesis discussion to assess your risk factor.
Does Having a Hysterectomy Make You Age Faster?
As hysterectomy, especially radical hysterectomy with the removal of ovaries, significantly reduces your estrogen production, you will experience surgical menopause immediately after the surgery, regardless of your age. Once in menopause, many women report seeing differences in their skin as soon as a few months or years post-procedure.
Studies have also shown that there are risks for rapid bone density loss, increased probability of fractures, as well as homeostasis endangerment – once estrogen is removed from your body, your body is put under stress until new homeostasis is established.
Like any other stressor, surgical menopause and hysterectomy can speed up the aging of your body. Luckily, there are treatments that can partially restore your estrogen levels and significantly slow down aging and the onset of all other post-hysterectomy aging symptoms. Certain foods rich in phytoestrogens can also significantly reduce the severity of menopause symptoms, such as hot flashes and mood swings.
Rapid Aging After Hysterectomy
Although hysterectomy itself does not cause rapid aging, it can do so if it is done with a joint procedure of oophorectomy – the removal of the ovaries. It is the removal of the ovaries that can cause rapid aging, especially as they produce estrogen. Without it, some bodily functions cannot be performed – ovulating is a great example. With this in mind, let’s consider what can happen if you have a radical hysterectomy and oophorectomy:
Estrogen Loss
Bilateral oophorectomy (the removal of both ovaries and Fallopian tubes) leads to severe estrogen loss. An essential sex hormone, estrogen regulates your ovulation and sex drive and can influence your body image. This means that you can experience loss of libido, no more periods, infertility, and other conditions.
There seems to be a correlation between the age of the hysterectomy with oophorectomy and the onset of these symptoms.
Namely, studies have shown that the younger the age when the procedure is done, the higher the likelihood for conditions connected to rapid aging to develop. The study included women under 46 years of age, and a total of 18 chronic conditions were considered together. The study has also shown that the onset of these conditions had no connection to the reason hysterectomies were performed.
Cognitive Impairment
Cognitive impairment or cognitive decline in women who have had a hysterectomy is a controversial topic. While many negate the connection, studies have proven that some form of cognitive decline or cognitive aging can be expected in women who have undergone hysterectomy. The decline increased with the complexity of the procedure:
- Women who have had hysterectomy alone had increased chances for cognitive decline,
- Women who have had a hysterectomy and unilateral oophorectomy had increased chances for cognitive decline compared to the first group,
- Women who had had a hysterectomy and bilateral oophorectomy had an even higher chance for cognitive decline compared to the women in both previous groups.
Bone Density Loss
Bone density loss is a pronounced condition generally experienced as a part of aging. The loss of bone material targets women predominantly, while some bone loss can also be experienced by men as they age. It is important to note that post-hysterectomy, women were more prone to bone density loss at a younger age. It also goes without saying that chances for related injuries, such as bone or vertebral fracture.
Older Appearance and Skin
The connection between hysterectomy and skin aging is not understood completely, although many women report that they can see a change in the quality of their skin. As it goes, hysterectomy procedures affect metabolic functions, which in turn may reduce the youthful appearance of the skin. Issues such as reduced elastin and collagen production may be culprits behind the rapid aging after hysterectomy.
Other Health Issues
Besides these, hysterectomy has also been connected to other chronic or acute medical symptoms and conditions. Here is a shortened list of what to expect after a hysterectomy:
- Coronary Artery Disease,
- Depression,
- Arthritis,
- Chronic Obstructive Pulmonary Disease,
- Osteoporosis,
- Irritability,
- Bone fractures,
- Difficulty sleeping,
- Hot flashes,
- Mood changes,
- Reduced libido,
- Painful intercourse,
- Night sweats,
- Incontinence, and
- Difficulty urinating.
Early Menopause – Surgical Menopause After Hysterectomy
Even if you do not have an oophorectomy with your hysterectomy, you should know that a number of women experience ovarian failure within five years of their hysterectomy. This means that surgical menopause can happen even when your uterus alone is removed.
It is for this reason that around 78% of women who have hysterectomy decide to have an adjunct removal of the ovaries. To offset the symptoms of menopause, such as hot flashes, mood swings, and night sweats, many women decide to start hormone replacement therapy after a hysterectomy.
HRT After Hysterectomy – Hormone Replacement Therapy
In this case, you will be taking hormones to substitute for the hormones that your ovaries have been producing. It can be very difficult for your doctor to exactly match the hormone replacement therapy to your exact ratio of estrogen and testosterone – for this reason, you may want to try different brands and different hormone ratios. However, if you are in a risk group for certain types of breast cancer, you may want to ask your doctor whether you should be taking HRT or not.
Hysterectomy FAQs
How Do You Slow Down Aging After Hysterectomy?
Taking hormone replacement therapy and staying physically active can prove very beneficial to slowing down aging after a hysterectomy. While the HRT is not suited for everyone, you should still try to stay physically active, as this will keep your joints and bones stronger. Adjusting your diet also has many benefits for hysterectomy patients.
Does Your Skin Change After Hysterectomy?
Many women experience changes in their skin after hysterectomy. The connection between the two may be indirect: hysterectomy may introduce some chronic conditions to your overall health, making your body age faster overall. You should consult with your family doctor about diet, exercise regime, and any supplements you may need to take to slow down skin aging.
Does Removing Ovaries Cause Aging?
Removing ovaries may contribute to your aging faster. Removing ovaries means removing the source of both estrogen and testosterone from your body, resulting in temporary stress while your body is recovering and possible chronic conditions. However, with hormone replacement therapy and other supplements, you may significantly slow down post-hysterectomy aging. Furthermore, new medicine may remove the need for ovaries removal, leaving the procedure for cancer-risk patients only.
Can you Get Osteoporosis After a Hysterectomy?
Hysterectomy does not cause osteoporosis. However, 26% of women will experience ovarian failure within five years post-hysterectomy, inducing premature menopause. This, in turn, may increase the chances for related chronic conditions, including bone density loss and osteoporosis.
Final Considerations
Hysterectomy is a surgical procedure in which the uterus and/or cervix and ovaries are removed from your body. As your ovaries produce estrogen and testosterone, it is possible that your body will need a long time to adjust to life without these hormones.
As many women report aging faster, as well as the development of some chronic conditions, it is safe to say that there is a connection between hysterectomy and faster aging. You should consult your family doctor about any concerns that you may have about hysterectomy and rapid aging.