Caregivers, family members, and even the afflicted seniors themselves struggle to understand the difference – delirium vs dementia. These medical terms get tossed around (among many other terms) with an onslaught of other information when people are seeing primary care physicians or geriatricians for new signs of confusion in seniors.
Is the person suffering from delirium or dementia? And if it’s delirium – which type? If it’s dementia – which type?
While they may have similar symptoms, the two are different. Delirium comes on quickly whereas dementia develops slowly over time. Delirium primarily affects attention whereas dementia primarily affects memory. Both are cognitive disorders.
If you have an elder parent or loved one who is showing signs of confusion and you take them to a hospital or health care provider, it’s possible that delirium could be misdiagnosed as dementia. In fact, it is not uncommon for any health care provider meeting a confused senior to assume dementia has set in.
Let’s dig a bit further.
What is Delirium?
Delirium is a common and preventable condition that can sometimes be life-threatening. It usually sets in rapidly, over the course of a few hours or days, and it can last for days or possibly months. People experiencing delirium may feel confused and have an altered perception of reality. In addition to physical symptoms, like headaches and drowsiness, delirium can cause people to become aware of memories, strong emotions, or disturbing thoughts.
3 Types of Delirium
There are three primary types of delirium: hypoactive delirium, hyperactive delirium, and mixed delirium.
- Hypoactive delirium
Hypoactive delirium means the person is underactive, slowed down, and possibly unresponsive. Lack of movement is one important sign of hypoactive delirium. Physicians often overlooked this time of delirium, which can be concerning since hypoactive delirium can indicate progressively poor health. Among those people who have dementia, those with hypoactive delirium were significantly more likely than those with hyperactive delirium to die within six months.
- Hyperactive delirium
Hyperactive delirium means the person is overactive. Hyperactive delirium is characterized by agitation, constant motion, and restlessness.
- Mixed delirium
Mixed delirium is a mix of both hyperactive and hypoactive symptoms.
Causes
Delirium can be caused by a number of conditions. It’s more common in older people and people who are hospitalized. In fact, delirium is probably the most common psychiatric condition experienced by older, hospitalized patients. “Hospital delirium” affects about 60% of people over age 75 who live in nursing homes. The risk for developing delirium increases when people are on dialysis, take multiple medications, or are being treated for more than one illness.
Age isn’t the only risk factor for delirium. Other high-risk populations include:
- People living with human immunodeficiency virus (HIV)
- People living with cancer, Parkinson’s disease, or chronic liver disease
- People have had a stroke
- People with dementia
Unfortunately, delirium also tends to extend hospital stays, slowing recovery. People with delirium face an increased risk of falls, dehydration, and infection, so it’s important to routinely screen older patients for delirium.
Symptoms
Symptoms of delirium usually set in rapidly, within a few hours or days. The most common symptoms of delirium are confusion and distress. People with delirium may also experience:
- Anxiety/fear
- Apathy
- Attention problems
- Lack of responsiveness
- Feeling disoriented
- Slower or reduced movement
- Incoherence (saying things that don’t make sense)
- Restlessness
- Delusions (false beliefs that conflict with reality)
- Hallucinations (seeing or hearing things that don’t exist)
- Insomnia or changes in sleep patterns
Some nurses measure these symptoms using what’s known as the Delirium-O-Meter, or D-O-M. The Delirium-O-Meter is a behavioral rating scale that helps care teams monitor the severity of delirium in geriatric patients.
Treatment
Treatment starts by identifying and addressing the underlying cause of the delirium. This may require changes to a person’s medications, for example. Sometimes antipsychotics may be used to reduce agitation. A safe and supportive environment is also important to treating delirium.
Can an Elderly Person Recover from Delirium?
Delirium often has a poor outcome for elderly people, which is why it’s important that physicians recognize the symptoms early on. Nurses and doctors are less likely to recognize symptoms of delirium in patients who are over age 80, have vision impairment, or have dementia.
What is Dementia?
Dementia is a group of symptoms caused by an underlying disease. These symptoms include memory loss and personality changes. Dementia tends to progress slowly over time.
Causes
Dementia is typically caused by an underlying disease like Alzheimer’s, Lewey Body, Huntington’s, or Parkinson’s, which damages or destroys nerve cells in the brain. Strokes can also cause dementia by reducing the blood supply to the brain. This is called vascular dementia.
Another notable cause of dementia is traumatic brain injury, or TBI. This is caused by repetitive head injuries, like injuries from boxing or playing football.
Some risk factors for dementia can’t be changed. These include:
- Age
Older people are at a higher risk of developing dementia. However, dementia can occur at any age.
- Family history
People with a family history of dementia are at a greater risk of developing the condition. But family history doesn’t guarantee a person will develop dementia. Similarly, lack of a family history doesn’t mean someone will not develop dementia.
- Down syndrome
People with Down syndrome have an increased risk of developing Alzheimer’s disease. In fact, about 50% of people in their 60s who have Down syndrome also have Alzheimer’s.
Luckily, some risk factors for dementia can be influenced. For example:
- Alcohol use
- Smoking
- Exercise
An active lifestyle can help reduce the risk of dementia. Diabetes, high blood pressure, high cholesterol, heart disease, and obesity are all risk factors that can be managed with exercise.
- Diet
A healthy diet is important to minimizing the risk of dementia, especially vascular dementia. People who aren’t getting enough vitamin D, vitamin B-6, vitamin B-12, or folate are at a higher risk of developing the condition. Meanwhile, diets that limit consumption of red meat, cheese, sweets, fried foods, and other high-saturated-fat foods demonstrate the protective effects on cardiovascular conditions that can result in dementia. Eating green leafy vegetables, nuts, and berries may also improve memory and slow cognitive decline.
Symptoms
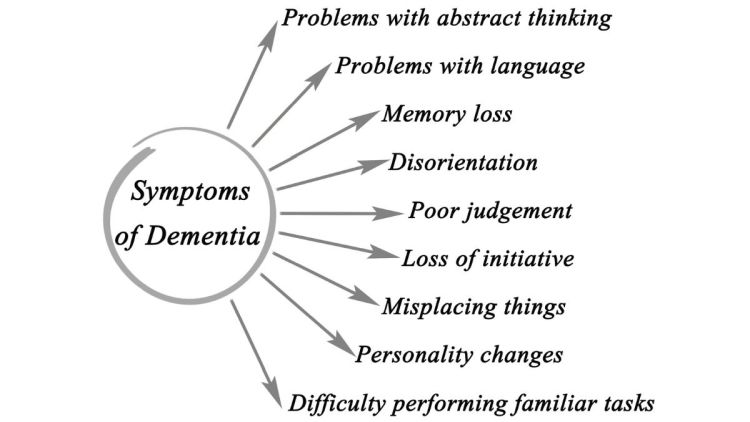
Symptoms of dementia vary depending on which portion of the brain is damaged. People may experience psychological changes, like personality changes, inappropriate behavior, depression, or anxiety. They may also experience cognitive changes, like memory loss, difficulty communicating, poor coordination, and diminished spatial abilities.
Treatment
Treatment depends on the underlying cause of the dementia. For example, dementia caused by Alzheimer’s disease is typically treated with symptomatic therapy.
Medications designed for Alzheimer’s can temporarily treat cognitive symptoms. Cholinesterase inhibitors, like Aricept, are a type of drug that boosts communication between brain cells. This tends to modestly improve symptoms. However, cholinesterase inhibitors may also cause diarrhea, nausea, loss of appetite, and sleep disturbances that affect quality of life.
Another drug, often used in conjunction with cholinesterase inhibitors, is Memantine. Memantine, also sold as Namenda, slows the progressions of symptoms in moderate or severe Alzheimer’s. However, it can cause dizziness and confusion in rare instances.
Treatment for vascular dementia focuses on managing the underlying health conditions that caused the dementia, like high blood pressure, high cholesterol, or high blood glucose levels. Treatment may comprise of increased exercise and changes to one’s diet, along with medicines like low-dose aspirin or anticoagulants.
For anyone with dementia, therapy and palliative care can make life easier for patients and their families. Physical therapy, speech therapy, and occupational therapy help people navigate activities of daily living. Meditation, music, and dance help with relaxation and improve cognitive function.
Can an Elderly Person Recover from Dementia?
Some causes of dementia are potentially reversible, like drug toxicity, depression, and metabolic causes. But for most patients, dementia is progressive and degenerative. While it’s possible for temporary fluctuations in symptoms to occur, improvement is not usually part of the natural progression of the condition.
3 Big Differences Between Delirium and Dementia
There are three major differences between delirium and dementia that every caregiver should know.
- Onset
Delirium is a rapid-onset condition, while dementia is a slow-onset condition. Delirium sets in quickly and lasts up to a few months at most, while dementia gets progressively worse over time and often is considered terminal.
- Symptoms
Delirium symptoms tend to fluctuate a lot, while dementia symptoms don’t. Delirium usually gets worse in the evening and improve in the day. On the other hand, people with dementia experience consistent impairment to their memory and thinking throughout the day. Additionally, delirium is mainly characterized by inattention, while dementia is characterized by memory loss.
- Treatment and prognosis
Delirium is reversible and can be managed with medication, while dementia is generally irreversible and is treated with symptomatic therapies and palliative care.
Delirium vs Dementia Summary
Delirium and dementia may present outwardly in some similar ways, but they are not the same thing. If you are wondering what you or a loved one has, the only real answer can be determined by speaking with a physician who specializes in diagnosing and treating these health conditions.